Brain Aneurysm
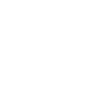
A brain aneurysm is an outward bulging or ballooning of a weak spot in the wall of an artery that supplies blood to the brain. Although they do not always break but in some cases they may rupture or leak, releasing blood into the brain and causing a hemorrhagic stroke that may cause brain damage or even death.
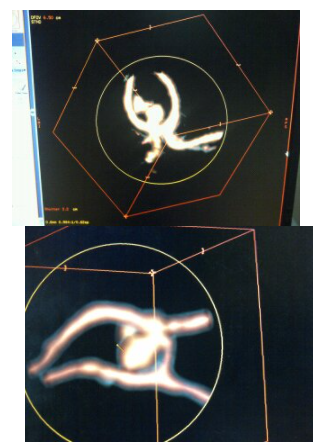
Location of Brain Aneurysm
The network of blood vessels at the base of the brain called the circle of Willis
Causes of Brain Aneurysm
Aneurysms have a variety of causes including:
- High blood pressure
- Atherosclerosis
- Trauma
- Heredity
- Abnormal blood flow at the junction where arteries come together
- Infections of the artery wall
- Brain tumors
- Drug abuse, especially cocaine
Symptoms of Brain Aneurysm
Generally most of the cases of brain aneurysm show no symptoms and may go unnoticed until some diagnostic tests are performed for other illness. In other cases, the symptoms depend upon rupture or unruptured state of aneurysm.
Symptoms of Ruptured Aneurysm
- Severe, sudden and unbearable headache that is different from past headaches and has never occurred before in life
- Neck pain & stiffness
- Nausea & vomiting
- Loss of sensations
- Fainting or loss of consciousness
- Double or blurred vision
- Sensitivity to light
- Pain above and behind the eye
- A dilated pupil
- Seizures
Symptoms of Unruptured Aneurysm
- Severe headaches
- Blurred vision
- Neck pain
- Fatigue
- Loss of balance and coordination
- Short-term memory difficulty
- Decreased concentration
- Perceptual problems
- Sudden changes in behaviour & speech
- Thinking or processing problems
Diagnosis of Brain Aneurysm
Early diagnosis of brain aneurysm prevents rupturing of the vessels and involves the following:
- Complete history of the patient
- Thorough physical & neurological examination
- CT scan
- umbar puncture
- Angiography
- MRI scan
- Cerebral angiogram
Brain Aneurysm Treatment
A section of your skull is removed to locate the aneurysm and a metal clip is placed on the opening of the aneurysm to cut off the blood flow. Your skull is then sealed shuted.
Endovascular coiling: Endovascular coiling doesn’t require any surgery that opens the skull. Surgeon will insert a catheter into your groin to reach the affected blood vessel where the aneurysm is located and will send tiny platinum coils through these tube and place them inside the aneurysm. Such coils conform to the shape of the aneurysm, stopping the blood flow there. This may be safer than surgical clipping, but it has a higher chance of the aneurysm bleeding again.
Flow diverter surgery: This Flow diverter surgery is for larger brain aneurysms in which neither clipping nor coiling would work. In such procedure, surgeon inserts a stent, usually made of metal mesh, inside the artery. It becomes a wall inside these vessel to divert blood away from the aneurysm.


 Request an Appointment
Request an Appointment Request Online Consultation
Request Online Consultation Enquiry form
Enquiry form