Trigeminal Neuralagia
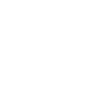
Trigeminal neuralgia or tic douloureux is a chronic pain condition that affects the trigeminal nerve in the face. The nerve carries sensations from face to the brain. The condition initially causes a jolt of excruciating pain that is intermittent, short and mild but can progress and cause longer, more-frequent bouts of searing pain.
Triggering factors of Trigeminal Neuralgia
Mild stimulation of face by any of the following can trigger the pain of trigeminal neuralgia:
- Brushing teeth
- Shaving
- Touching or washing face
- Putting on makeup
- Chewing
- Biting
- Swallowing
- Talking
- Drinking
- Smiling
Causes of Trigeminal Neuralgia
Trigeminal Neuralgia is caused by a disruption in the functioning of the trigeminal nerve. In most of the cases it occurs when a normal blood vessel (artery or vein) presses against the trigeminal nerve at the base of the brain. This pressure on the trigeminal nerve causes it to malfunction.
Other than this, following may also cause trigeminal neuralgia:
- Aging as it is more likely to occur in people who are older than 50
- Multiple sclerosis or similar disorders that damage the myelin sheath protecting certain nerves
- Brain lesions or other abnormalities
- Tumor compressing the trigeminal nerve
- Surgical injuries
- Stroke
- Facial trauma
- Sometimes the cause remains unknown
Symptoms of Trigeminal Neuralgia
The symptoms of trigeminal neuralgia may include one or more of the following patterns:
- Sudden, severe & stabbing facial pain that may last from a few seconds to several minutes
- Pain may feel like an electric shock in areas supplied by the trigeminal nerve including around the cheek, jaw, teeth, gums, lips, or less often the eye and forehead
- Usually the pain is localized to one side of the jaw or cheek but in some cases, it may occur at different places and at different times
- Frequency of attacks may vary from 1 or 2 per day to almost 12 per hour reaching up to hundred times per day
- Constant aching, burning feeling that’s less intense than the spasm-like pain
Diagnosis of Trigeminal Neuralgia
There are no specific tests to accurately determine the certainty of the condition and can mainly be diagnosed based on the description of symptoms specified by the patient including type, location and trigger of pain. Apart from this, following examinations and diagnostic tests may help the physician to diagnose the condition:
- A thorough physical and neurological examination
- MRI scans in cases where trigeminal nerve is irritated due to tumor or multiple sclerosis, can be used to diagnose trigeminal neuralgia
Treatments
Medications
• Anticonvulsant drugs. Carbamazepine is one of the first choice for treating pain associated with Trigeminal Neuralgia. Our healthcare provider may also prescribe other Anticonsultant drugs including Oxcarbazepine, phenytoin, Lamotrigine, sodium valproate, gabapentin, clonazepam &topiramate and many more. If you have been taking one of these medications and feel that it isn’t helping as it should, you can ask your doctor to increase specific dose or you can try another form of medication. While these anticonvulsant drugs can help relieve pain, the side effects may be including dizziness, nausea, confusion and drowsiness.
• Tricyclic antidepressants. Amitriptyline or Nortriptyline are the common medications in this category, and they are generally used to treat Type 2 trigeminal neuralgia symptoms.
• Muscle relaxants. Baclofen can be used alone/together with the carbamazepine or phenytoin.
• Other medications. A Botulinum toxin injection is used to block sensory nerves. In some instances, nerves block is used to provide temporary relief.
Surgery
If you don’t have response to any of these medications or believe your condition is worsening over time, you could be a candidate for surgery. You have a several surgery options. Specific doctor may likely recommend one for you based on the severity of pain, your preference, your physical health, previous surgeries and the surgery related risks and benefits. Additionally, it is more difficult to perform surgery on those suffering from Type 2 trigeminal neuralgia.
Percutaneous (through the skin) surgical techniques include:
• Balloon compression. The surgeon will insert a tube, called a cannula, through your cheekup to the trigeminal nerve. From these, they insert a catheter with a small balloon through the tube. They inflate the balloon, compressing the nerve and damaging the pain-causing fibers. Balloon and catheter are removed at the end of the procedure. This procedure has been known to relieve symptoms for 1-2 years, though it can cause some numbness in the face.
• Glycerol injection rhizotomy. The surgeon will inject glycerol through a needle into the nerve center, right where it splits into 3 branches. By injecting these glycerol into the root of the trigeminal nerve, it causes selective nerve damage that disrupts the body’s ability to transmit pain signals to the brain. This procedure can suppress pain for 1-2 years, though it can be performed multiple times. Such procedure can also cause some facial numbness, as well as tingling.
• Radiofrequency thermal lesioning. The surgeon will insert a needle through your cheek, all these way through to the base of your skull, which is then used to send an electrical current to identify the specific pain point on the trigeminal nerve. The heat is applied to the nerve until a lesion forms, destroying some of the nerve fibers. About half of patients WHO options for this procedure see their symptoms return after 3 to 4years. You may also feel facial numbness as a result of this procedure.
Microvascular decompression is a more invasive surgical procedure. It is typically the most successful of all these procedures, as it can provide pain relief for up to 10 years. The goal of this procedure is to provide a long term solution, where the trigeminal nerve can recover and return to a more normal, pain-free state. However, it is invasive because the surgeon must create an opening behind the ear, thus exposing the trigeminal nerve root. This opening reveals the blood vessel that may be compressing the nerve; once your surgeon identifies the specific blood vessel, a cushion is placed between the nerve and the blood vessel. Newer patients who are otherwise in good health are suitable candidates for this procedure.
If a surgeon attempts to perform microvascular decompression but doesn’t find a blood vessel actively pressing against the nerve, neurectomy might be performed. In this procedure, surgeon cuts either part of the nerve near the brain stem or some of the nerve’s branches in the face. The neurectomy can have lasting side effects, including numbness in the areas where the surgeon cuts part of the nerve & impaired hearing. Nerves in the face, however, can grow back over time, meaning the pain will return in that specific area as well.
Stereotactic radiosurgery uses Gamma Knife, Cyber-Knife or LINAC surgery to deliver a highly concentrated amount of radiation on the trigeminal nerve root, where it meets the brain stem. After this procedure, a lesion will form on the nerve that will disrupt its ability to transmit pain signals to the brain, though you may increasingly feel numbness in your face as a result. It can be a few weeks before you begin to see the effects of this procedure. Stereotactic radiosurgery generally eliminates symptoms for about 3 years.
Related Videos :


 Request an Appointment
Request an Appointment Request Online Consultation
Request Online Consultation Enquiry form
Enquiry form